A recently published special issue of nanomaterials explores the recent advances related to nano-engineered strategies for biomaterials and implants in bone tissue engineering. Novel nano-engineering strategies are showing promising results with regard to enhanced osteogenesis at the implant/biomaterial and bone tissue interface. Also, nano-fibrous scaffolds produced from natural and synthetic materials have shown promise in promoting bone formation.
Biomaterial research on bone regeneration has advanced its focus from macro- and micro- properties to nano-scale characteristics that mimic the host tissue biology.
Nano-engineered biomaterials exceed the bone regeneration and linking performance of conventional macro- and micro-scaled biomaterials. Resorbable biomaterials, Extracellular matrix (ECM)-mimicking nanofibrous scaffolds, and nanoscale modified non-resorbable metal-based implants have shown remarkable outcomes.
Leading scientists worldwide have contributed to a total of 8 original research and review papers that show how novel nano-engineering strategies hold great potential in bone tissue engineering.
Some salient points from the current research:
- Hydroxyapatite (HA) is biocompatible and non-immunogenic and has been widely used as a scaffold or towards surface modification for biomaterials or implants. Inorganic nanomaterial-based therapy focuses on nano hydroxyapatites, nano-silica, and metallic nanomaterials to increase biomineralization and bone defect repairing.
- Biomimetic HA may be effective at advancing osteogenesis and mechanical strength, but tissue volume remains challenging. This issue was addressed in an in-vitro study. The results showed that the composite maintained the hydrogel volume and increased the cell viability and bone differentiation ability. Biomimetic and biogenic Hydroxyapatite (HA) based nanomaterials have promising bone regeneration applications.
- Human teeth-derived bioceramics showed no adverse effects and had good adherence to human alveolar stem cells. Furthermore, the bioceramic-treated defects in mice calvaria resulted in accelerated vascularization, demonstrating the capability of such biomaterials in bone regeneration.
- 3D fibrous scaffolds enable cellular interaction through nanoscale focal adhesion complexes. The primary human osteoblast sensing and responses to polycaprolactone (PCL) fibrous 3D scaffolds caused immature vinculin focal adhesion formation and decreased the nuclear localization of the mechanosensor-yes-associated protein (YAP). Moreover, when aligned fibers compared to random fibers, they elongated the cell and nucleus shape and activated global DNA methylation.
- Ti-based implants are bioinert, and in patients with poor bone quality /quantity, increased bioactivity performance is needed to harmonize osteogenesis. Therefore, surface modification of Ti-based implants using various topographical, chemical, biological, and therapeutic strategies in the macro-, micro-, and nano-scales have been performed. Results showed nano-engineered Ti implants have surpassed macro-and micro-scale implants by attaining appropriate bioactivity and therapeutic performance.
- Surface characterization and cell response evaluation (MC3T3-E1 osteoblast-like cells) in vitro research confirms the influence of incorporating bioactive agents, such as HA and Mg particles, onto Ti implants for inducing bone formation.
- Cost-effective TiB-reinforced alpha Ti matrix composite (TMC) characterization revealed an increase in hardness, modulus, and hardness to modulus ratio. Thus, it is confirmed that TMC has an excellent performance in biomedical implant applications.
This is the summary of a special editorial by Dr. Karan Gulati, Dr. Abdal-hay, and Dr. Ivanovski that talks about recent advancements in nano-engineered biomaterials for bone tissue engineering. This editorial was published in the Special Issue "Novel Nano-Engineered Biomaterials for Bone Tissue Engineering" of Nanomaterials. This special issue covers the current nanotechnology advances, clinical translation challenges, and prospects, enclosing both resorbable polymeric and non-resorbable metallic biomaterials that enable controlled and customized organization of osteogenesis at the biomaterial–bone interface.
Tags:
Finally, researchers have succeeded in designing artificial enamel, which seems to have much better mechanical properties compared to natural enamel –...
Silver nanoparticles (Ag NPs) are one of the most unique nanotechnology-based products among all metallic nanoparticles. In this article, Dr. Aditya K. S. ...
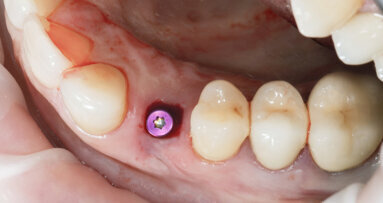
BRISBANE, Australia: Ensuring the formation of a solid soft-tissue seal at the dental abutment surface is crucial for protecting the underlying tissue from ...
KARLSRUHE, Germany: Micro- and nanotechnology are gaining importance in the medical field and particularly in implantology. Dental implants provide a great ...
GOTHENBURG, Sweden: Large cranial reconstructions are being increasingly performed worldwide, but remain a substantial clinical challenge. Researchers from ...
Live webinar
Tue. 26 May 2026
9:30 pm IST (New Delhi)
Live webinar
Tue. 26 May 2026
11:30 pm IST (New Delhi)
Live webinar
Wed. 27 May 2026
5:30 pm IST (New Delhi)
Live webinar
Thu. 28 May 2026
9:30 pm IST (New Delhi)
Dr. Anthony Viazis DDS, MS. Inventor & Founder of Fastbraces®
Live webinar
Mon. 1 June 2026
10:30 pm IST (New Delhi)
Live webinar
Wed. 3 June 2026
10:30 pm IST (New Delhi)
Live webinar
Thu. 4 June 2026
11:30 pm IST (New Delhi)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East














































To post a reply please login or register