BUDAPEST, Hungary: Studies have shown that the implant surface roughness influences the degree of biological integration and success rates of dental implants, which has resulted in a shift of focus from machined to roughened implant surfaces. However, clinicians have still been looking for strong scientific evidence that supports the use of sandblasted implants over machined ones in clinical practice. Looking at this need, the team of researchers from the Semmelweis University in Budapest, carried out a comparative evaluation of implant failure and marginal bone loss between the two types of surfaces.
Ever since it emerged that surface roughness greatly influences the degree of biological integration and success rates of dental implants, various surface modifications such as sandblasting, acid-etching, anodization, plasma-spraying, coating with different bioactive surfaces and the combination of these have come into practice.
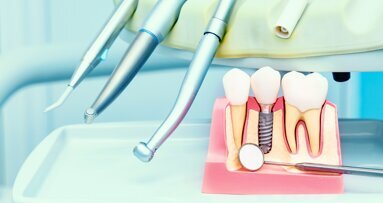
Among all these methods, sandblasting was the earliest to be introduced, during which, ceramic particles such as titanium oxide, aluminium oxide or silica are blasted on to the implant surface. Two factors - the sand particle size and the speed with which they hit the implant surface – play a key role in influencing the implant surface roughness. Compared to the machined implants that have smoother surfaces with shallow grooves, the sandblasted ones demonstrate irregular, rough surfaces.
Studies have shown different results while demonstrating the effects of sandblasting on osseointegration, While several in vitro studies have demonstrated the positive effects of sandblasting on osseointegration, some preclinical and clinical studies have shown that moderately rough surfaces may not perform better.
These studies bring in a newer perspective to osseointegration by shifting the focus to the formation of biofilm. They suggest that a rougher surface may influence the process of biofilm formation, making it easier for the bacteria to attach to the implant surface. The bacterial biofilm renders the implants vulnerable to peri-implantitis, resulting in marginal bone loss around the rough surfaces.
The current study was a systematic review, which included seven studies, comparing 362 sandblasted surfaces with 360 machined ones. The results showed that after one year of use, the risk of failure among sandblasted surfaces was 80 per cent lower when compared to machined implants. When the effect of sandblasting was evaluated after five years, the risk of failure was 74 per cent lower in the sandblasted implant surfaces. However, when marginal bone loss was assessed, there was no significant difference between the two implant surfaces after one and five years of use.
The researchers concluded: “This meta-analysis reveals that sandblasting is superior over machined surface in implant failure but not in marginal bone level in healthy subjects. It also points out the need for further randomised clinical trials with large sample size for objective determination of the clinical benefits of certain implant surface modifications.”
The study was conducted in collaboration with the University of Pécs and the University of Szeged, both in Hungary.
The study, titled “Sandblasting reduces dental implant failure rate but not marginal bone level loss: A systematic review and meta-analysis”, was published online on 3 May 2019 in PLOS ONE.
Tags:
ZURICH, Switzerland: Clinical evidence has established dental implants as a great treatment option to replace missing teeth. However, even with the high ...
Machine Learning (ML) is a marvel of change in healthcare; it has changed the way medical professionals diagnose, treat, and manage diseases. Imagine a ...
Artificial intelligence (AI) and machine learning (ML) have emerged as powerful tools for improving diagnosis, treatment planning, and patient monitoring in...
Dynamic navigation delivers superior accuracy and safety in maxillary implant placement. A recently published split-mouth study shows marked reduction in ...
SEOUL, South Korea: Dental implants are a key treatment for tooth loss, but can cause a variety of complications. One such complication is osteonecrosis, ...
The digital revolution continues. Like all areas of dentistry, implantology is going digital. The potential benefits of a digital workflow can be applied to...
According to the latest research from IIT Bombay, masks and PPE materials with hydrophilic surfaces could help the respiratory droplets dry faster, thus ...
KUALA LUMPUR, Malaysia: Investigating the plaque-inhibiting effect of a green tea and miswak mouthwash, researchers from the University of Malaya have found...
Implant study group (ISG) reached another milestone with the graduation of its 35th batch. For over 15 years, Dr. Girish Rao and Dr. Anandakrishna GN, ...
Leuven, Belgium: As digital dentistry continues to evolve, artificial intelligence (AI) is stepping into roles once thought to require exclusively human ...
Live webinar
Thu. 14 May 2026
9:30 pm IST (New Delhi)
Live webinar
Thu. 14 May 2026
11:30 pm IST (New Delhi)
Prof. Hani Ounsi DDS PhD FICD
Live webinar
Tue. 19 May 2026
8:30 pm IST (New Delhi)
Live webinar
Tue. 19 May 2026
10:30 pm IST (New Delhi)
Prof. Dr. med. dent. Ivo Krejci
Live webinar
Wed. 20 May 2026
4:30 pm IST (New Delhi)
Dr. Graham Carmichael BDSc (Hons), DClinDent (Pros), FRACDS, Dr. Robert Gottlander DDS
Live webinar
Wed. 20 May 2026
6:30 pm IST (New Delhi)
Live webinar
Wed. 20 May 2026
10:30 pm IST (New Delhi)
Prof. Dr. med. dent. Tim Joda PhD, MSc, eMBA



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



















































To post a reply please login or register