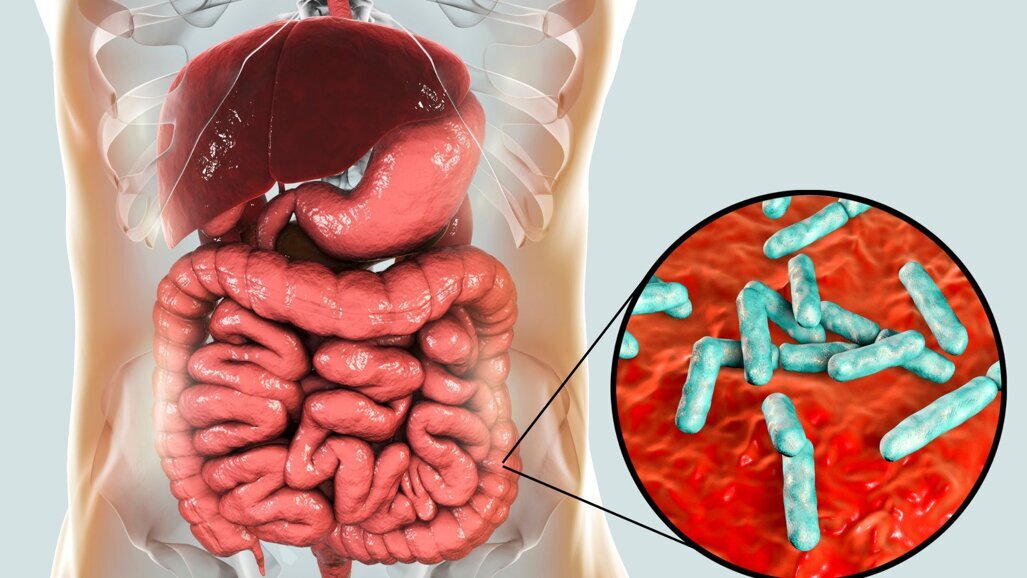
Potential pathways of gut translocation of oral pathobionts
The oral bacteria from the oral cavity can be translocated to the gut mucosa through the following two potential routes:
- Hematogenous spread
- Oral bacteria can spread systemically through a hematogenous route.
- Mechanical injuries in the oral cavity can result in the dissemination of oral bacteria into the systemic circulation.
- Hematogenously inoculated Fusobacteria strains are more thriving in colonization in the gut tumor than gavaged strains, implying the circulatory system plays a major route in oral bacteria dissemination.
- Oral bacteria can seize and remain inside dendritic cells and macrophages, indicating the hijacking of host immune cells to serve as Trojan horses for the spread of bacteria from the oral to the gut mucosa.
- Enteral dissemination
- An individual can swallow around 600 times a day and synthesize ~1.5 L of saliva containing 1.5x10^12 oral bacteria.
- More than half of the oral bacterial species have been detected in the gut, indicating oral–gut translocation of oral bacteria even in healthy people.
- Generally, oral bacteria poorly colonize in the healthy gastrointestinal tract (GIT) because of the multiple barriers conferred by the healthy gut.
- Gastric acidity is the first barrier against the translocation of oral bacteria to the gut mucosa.
- Oral bacteria translocation can also be observed in patients who have gastric achlorhydria, gastroesophageal reflux disease, and gastritis after gastric surgery.
- Various types of oral pathogens, like P. gingivalis, can survive in the acidic environment of the stomach and pass through the gut barrier.
- Thus, the prevention of the enteral transmission of oral pathogens is the primary defense mechanism.
- Secondly, maintaining the gut's harmonious microbial structure is crucial for avoiding ectopic colonization by ingested oral bacteria, since the gut resident microbiota confers resistance to colonization.
- Factors responsible for gut microbiota dysbiosis include gut inflammation, artificial sweeteners, diets, and antibiotic treatment.
Microbial routes of direct gut colonization by oral pathogens
Multiple oral pathogens that colonize the gut may induce abnormal immune responses in GIT, thus leading to intestinal inflammation. Following oral bacteria are majorly responsible for gut inflammation:
- Fusobacterium spp.
- The role of Fusobacterium spp. is still debatable in gut inflammation.
- F. varium and F. nucleatum can permeate the intestinal epithelium and induce the synthesis of proinflammatory cytokines.
- F. nucleatum can invade intestinal epithelial cells and promote the expression of proinflammatory cytokines.
- Additionally, F. nucleatum can disrupt the integrity of the epithelial barrier.
- Porphyromonas Gingivalis
- P. gingivalis is the main periodontopathic bacteria involved in the pathogenesis of periodontitis.
- Studies showed that the orogastric administration of P. gingivalis to mice can disrupt the integrity of the gut epithelium.
- Continuous administration of P. gingivalis to mice leads to endotoxemia, reduced gene expression of tight junction proteins, and increased proinflammatory cytokines in the gut.
- Staphylococcus aureus
- S. aureus is observed to adhere to intestinal epithelial cells.
- Oral administration of S. aureus strain RN8098 into antibiotic–penetrated mice produces epithelial damage in the small intestine.
- Klebsiella spp. and Enterobacter spp.
- Klebsiella spp. and Enterobacter spp. colonization have been isolated from the saliva of patients with Crohn’s disease, resulting in potent Th1 cell differentiation in the gut of gnotobic animals.
- Oral inflammation fosters blooms of Enterobacteriaceae, including Klebsiella spp. and Enterobacter spp., in genetically susceptible mice, leading to exacerbation of intestinal inflammation.
Conclusion
Over the last decade, the research area of intestinal inflammation and oral microorganisms has widely expanded by studies that have mainly focused on the effect of direct colonization of oral pathobionts in the gut. Moreover, the usage of murine models showed the novel aspects of the complicated intermucosal connection between the gut and the oral cavity.



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East













































To post a reply please login or register