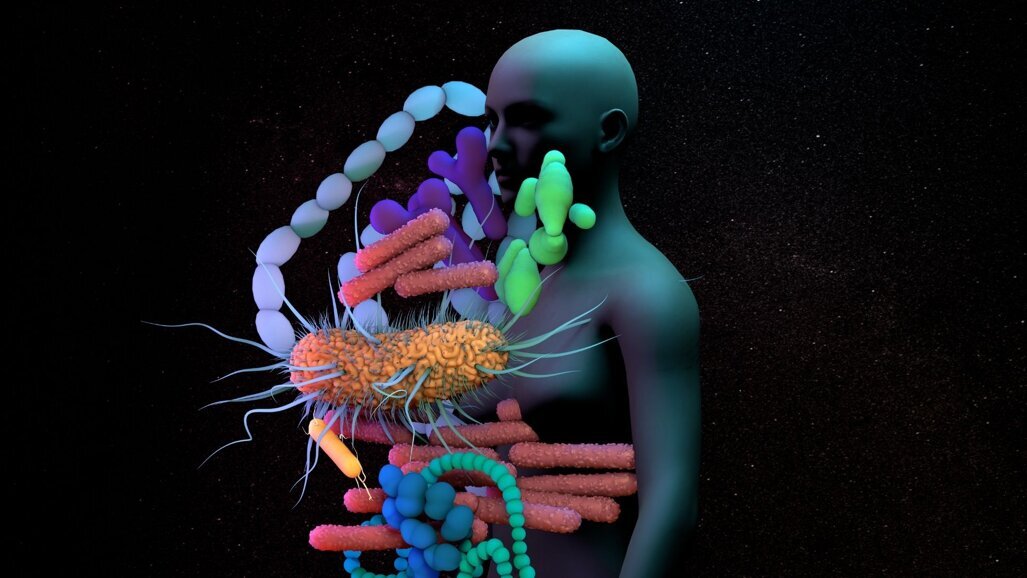
The human body consists of distinct and abundant microorganisms referred to as the microbiome [1]. The oral cavity is colonized by 700 different species of bacteria [2]. The unique oral microbiome niches are mucosal surfaces, tooth surfaces, and saliva [1]. The gut and oral microbiota are the largest and second-largest microbiota in the human being, respectively [3]. They are physically connected as the oral cavity is the beginning of the digestive tract, thus a large number of oral bacterial species can enter the gastrointestinal tract (GIT) through saliva. The alteration of oral and gut microbiota composition is known as dysbiosis. Recent evidence suggests that oral–gut microbiota dysbiosis plays a crucial role in modulating the initiation and progression of an array of autoimmune diseases. Therefore, targeting and reversing oral–gut microbiota dysbiosis can be an effective strategy for treating autoimmune diseases [1,4].
Oral microbiota targeted therapy
To prevent autoimmune diseases, it is important to maintain homeostasis dynamics between the oral microbiota, gut microbiota, and the host immune system. The driving factors that significantly affect the composition and structure of the oral microbial flora are poor oral hygiene, smoking, dietary shifts such as high carbohydrate, fat, and sugar intake, administration of antibiotics, and infections [1]. The main potential strategies for treating oral microbiota-mediated autoimmune diseases are:
Good oral hygiene
Oral infections such as dental caries and periodontitis upregulate several systemic inflammatory reactions which, in turn, play a crucial role in the initiation and development of many autoimmune diseases. Thus, maintaining oral hygiene can prevent autoimmune diseases [5].
Low carbohydrate, sugar, and fat diet
These dietary changes can reduce the oral microbial load, thereby affecting the composition of the oral microbial communities.
Healthy lifestyle
Lifestyle changes including proper sleep, stress reduction, and physical exercise can improve the condition of patients suffering from autoimmune diseases.
Usage of prebiotics, probiotics, or synbiotics
Probiotics are foods or supplements that contain live microorganisms intended to maintain or improve normal microflora. Prebiotics are typically high-fiber foods that promote the production of beneficial microbial metabolites for pathogenic bacteria suppression and improvement of the gut barrier [1]. For instance, Prebiotic D-tagatose suppresses the growth of the oral pathogens Streptococcus Mutans (S. mutans) and S. gordonii [1]. Synbiotics are mixtures of both probiotics and prebiotics that improve the activity and survival of beneficial gut microflora.
Oral Microbiota Transplantation (OMT)
Huang et al. suggested that OMT can be a promising strategy for the treatment of autoimmune diseases. Oral bacteria can be efficiently encapsulated for curing oral microbiota-mediated autoimmune diseases. A recent study demonstrated that OMT alleviated radiotherapy-induced oral mucositis by altering the oral microbiota composition in mice [1].
Nanomedicine–based therapeutics
The nanomedicine–based strategies involve biological immunomodulatory agents for the treatment of autoimmune diseases such as Inflammatory bowel disease (IBD), psoriasis, rheumatoid arthritis (RA), systemic lupus erythematosus (SLE), multiple sclerosis (MS), and type 1 diabetes (T1D). For instance, TNF – α siRNA nanomedicine-targeted macrophages can significantly reduce TNF – α levels to improve the condition of patients suffering from IBD [1].
Gut microbiota targeted therapies
The composition and function of the gut microbiota are generally altered in patients with autoimmune disorders [4]. The major potential strategies for curing gut microflora-mediated autoimmune diseases are:
Fasting-Mimicking Diet (FMD)
The FMD consists of specific plant-based ingredients such as low carbohydrates, proteins, and good fatty acids that keep the patient in a fasting state. This diet protects the body by rejuvenating the cells and improving their functions, thus reducing intestinal inflammation [4].
Water–only fasting intervention
This intervention can enhance the body’s regenerative mechanisms and also reduce inflammatory markers [4].
Probiotics and prebiotics
Probiotics might be used as an adjuvant therapy to maintain the homeostasis of the gut microbiota and can affect systemic immune responses. Prebiotics support numerous digestive and immune functions [4].
Fecal Microbiota Transplantation (FMT)
FMT is an effective therapeutic modality that can alter the composition of the gut microbiome in clinical settings. The process involves transferring the gut microbiota from a healthy donor, already screened for pathogens or any underlying disorder to a recipient through various modes like oral capsules, enemas, or transnasal intestinal tube infusion of bacterial fluids. Thus, it provides colonization resistance, produces favorable metabolites, and restores mucosal immune system interactions while improving the symptoms of the patient. Several clinical trials have been conducted to study the effects of FMT in different autoimmune diseases [6].
FMT and Rheumatoid Arthritis (RA)
A recent study on RA patients treated with FMT revealed that FMT can alleviate the symptoms of RA. On the 42nd day after FMT, the Health Assessment Questionnaire Disability Index (HAQ-DI) dropped to 0.05, the Disease Activity Score 28 (DAS28) was 1.9 from the initial score of 6.6, and the titer of the rheumatoid factor decreased to 158 from the initial value of 314 IU/ml [7].
FMT and Multiple Sclerosis (MS)
The latest study conducted on nine patients with MS who were treated with monthly FMTs for six months disclosed that the patients with abnormal intestinal permeability improved to the normal range. Additionally, the concentration of Hungatella hathewayi spp. also increased post – FMT, thus suggesting the efficiency of FMT in modifying the gut microbiome composition [8].
FMT and Inflammatory Bowel Disease (IBD)
In 2014, a meta-analysis of 122 patients revealed a potential impact of FMT in different types of IBD; pooled results from 18 studies showed a clinical remission of 36.2% and 60.5% in Ulcerative colitis (UC) and Crohn’s disease (CD) patients, respectively. Another clinical trial named Fecal Microbiota Transplantation in Ulcerative Colitis (FOCUS) on 85 active UC patients, evaluated the clinical and endoscopic remissions while comparing FMT by colonoscopy, FMT enema, and a placebo for eight weeks. A remission rate of 27% was observed in the FMT group while 8% remission was observed in the placebo groups [9].
Conclusion
The oral and gut microbiota dysbiosis plays a critical role in the initiation and progression of several autoimmune diseases, thus targeting oral and gut microbes can be a potential strategy for curing autoimmune conditions. The current approaches including dietary changes, probiotics, prebiotics, and FMT have improved the condition of patients suffering from autoimmune diseases. Further clinical trials are needed to study the effect of OMT and FMT therapies on autoimmune diseases.
References:
1. Huang X, Huang X, Huang Y, Zheng J, Lu Y, Mai Z, Zhao X, Cui L, Huang S. The oral microbiome in autoimmune diseases: friend or foe? Journal of Translational Medicine 2023; 21:211.
2. Lu M, Xuan S, Wang Z. Oral Microbiota: A new view of body health. Food Science and Human Wellness 2019;8:8-15.
3. Tan X, Wang Y, Gong T. The interplay between oral microbiota, gut microbiota and systemic diseases. Journal of Oral Microbiology 2023; 15: 2213112.
4. Mahajan P, Kulkarni A, Bandre A, Subramanian S, Mahajan S. Role of Gut Microbiota in Autoimmune Diseases. J Vaccines Immunol 2021; 6:163.
5. Julkunen A,Heikkinen AM, Söder B, Per-Östen Söder ,Toppila-Salmi Sand, Meurman J H. Autoimmune Diseases and Oral Health: 30-Year Follow-Up of a Swedish Cohort. Dent. J. 2018;6:1-7.
6. Sorbara, M. T., and Pamer, E. G. Microbiome-based therapeutics. Nat. Rev. Microbiol. 2022;20 (6):365–380.
7. Zeng J, Peng L, Zheng W, Huang F, Zhang N, Wu D, Yang Y. Fecal microbiota transplantation for rheumatoid arthritis: A case report. Clin Case Rep. 2020 Dec 23;9(2):906-909. doi: 10.1002/ccr3.3677. PMID: 33598269; PMCID: PMC7869316.
8. Al KF, Craven LJ, Gibbons S, Parvathy SN, Wing AC, Graf C, Parham KA, Kerfoot SM, Wilcox H, Burton JP, Kremenchutzky M, Morrow SA, Casserly C, Meddings J, Sharma M, Silverman MS. Fecal microbiota transplantation is safe and tolerable in patients with multiple sclerosis: A pilot randomized controlled trial. Mult Scler J Exp Transl Clin. 2022 May 11;8(2):20552173221086662. doi: 10.1177/20552173221086662. PMID: 35571974; PMCID: PMC9102167.
9. Colman RJ, Rubin DT. Fecal microbiota transplantation as therapy for inflammatory bowel disease: a systematic review and meta-analysis. J Crohns Colitis 2014;8:1569–81.
Tags:
In recent decades, we have recognized the vital role of microbiota in health and disease. The human gut and oral microbiota, the body’s largest ...
A growing body of evidence now links COVID-19 outcomes with vitamin D status. Subhasree Ray, a clinical and public health nutritionist, analyses the ...
AMSTERDAM, Netherlands: In recent years, increasing attention has been given to aspects of oral health in patients with rheumatoid arthritis (RA), ...
This guest editorial by Dr Sanjiv Hyoju talks about a possible connection between a diet-induced disturbance in the gut microbiome equilibrium and its ...
People that traditionally exhibit vitamin D deficiency, such as older adults and nursing home residents, are the same groups that have also been excessively...
PHILADELPHIA, U.S./CHENGDU, China: Periodontitis remains the sixth most prevalent infectious disease worldwide, and the most common cause of tooth loss ...
This guest editorial comes from Dr. Wenyuan Shi, Chief Scientific Officer and Chief Executive Officer of The Forsyth Institute – the only independent ...
OKAYAMA, Japan: Since periodontitis has been linked to systemic health conditions, including heart disease, diabetes, cancer and Alzheimer’s disease, ...
LONDON, UK/CHENNAI, India: UK Research and Innovation and India’s Department of Biotechnology in the Ministry of Science and Technology have recently ...
Live webinar
Wed. 3 June 2026
10:30 pm IST (New Delhi)
Live webinar
Thu. 4 June 2026
11:30 pm IST (New Delhi)
Live webinar
Mon. 8 June 2026
9:30 pm IST (New Delhi)
Live webinar
Mon. 8 June 2026
10:30 pm IST (New Delhi)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
11:30 pm IST (New Delhi)
Live webinar
Wed. 10 June 2026
8:30 pm IST (New Delhi)
Live webinar
Wed. 10 June 2026
11:30 pm IST (New Delhi)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East
















































To post a reply please login or register