Composite resins have been the choice of restorative material for more than 20 years. Most clinicians have mastered the layering protocol for anterior teeth but achieving life-like posterior restorations is still a struggle for many. This article discusses the cuspal build up technique to achieve predictable, aesthetic restorations while also overcoming the problems associated with polymerization shrinkage.
The restorative procedures of posterior areas are the most frequent in our daily practice. Despite the fact that composites have been used in posterior teeth for more than twenty years, there’s still a lot of problems associated with polymerization shrinkage due to which the success of direct posterior restorations was always questioned, let alone the aesthetics pertaining to posterior teeth.
Among several techniques described in the literature i.e oblique layering, incremental layering etc, the cuspal layering technique also known as a the pizza technique has claimed to reproduce the aspects of natural dentition, as well as to allow control of stress generated by polymerization shrinkage.In this technique each cusp is build one by one. As every cusp is built independently the natural anatomy is reproduced while layering thus reducing chair time. A major advantage of this technique is reduction of polymerization shrinkage. As only two walls are involved during one cusp build up the configuration factor is almost negligible and so is the polymerization shrinkage.
This article is based upon a case report to present the layering protocol and its results.
Case Report
A young 16-year-old girl entered the operatory with the chief complaint of pain in her lower left tooth. On radiographic and clinical analysis, tooth number 36 presented with a huge decay extending upto the pulp and the tooth required endodontic therapy. The patient also showed misaligned teeth and was suggested orthodontic treatment. The patient agreed for the same. As the tooth had sufficient amount (2mm) of enamel all around (the proximal walls and the buccal and lingual walls intact), the treatment plan devised was to do a direct composite restoration instead of cuspal coverage. This treatment would save a lot of tooth structure and increase the longevity of this tooth. This would also help the orthodontist to bond on to enamel rather than ceramic. The patient was informed that this restoration is an interim restoration and in future this tooth would require cuspal coverage.
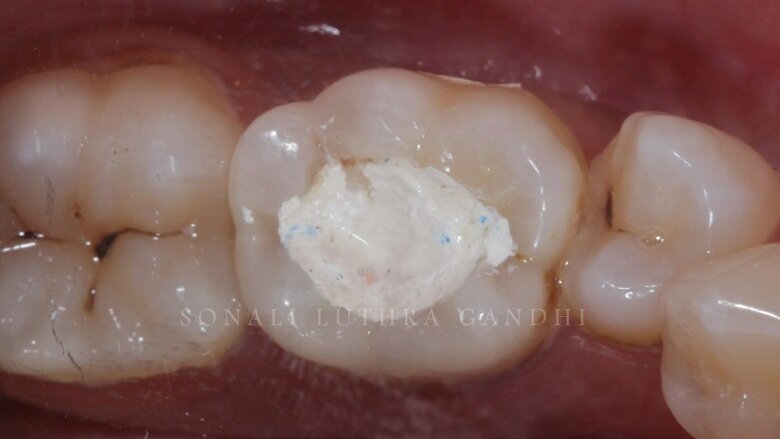
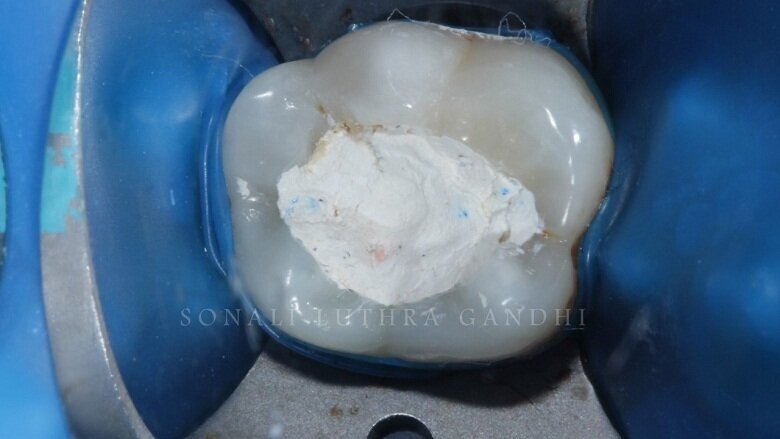
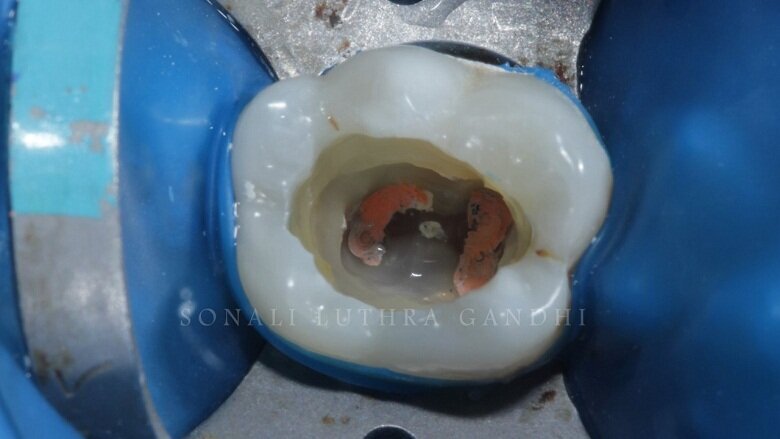
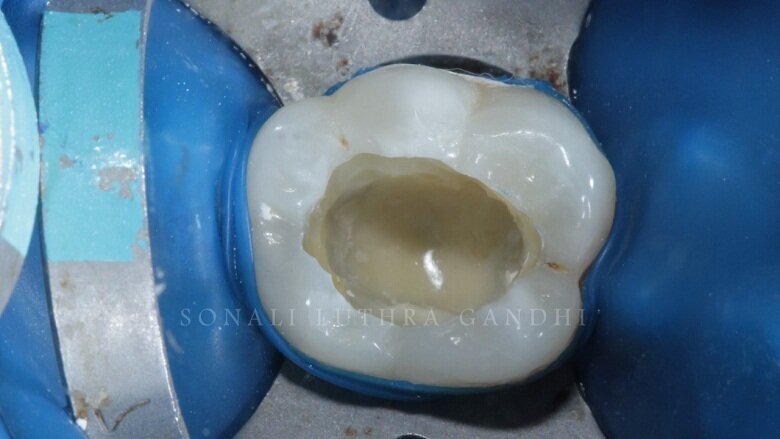
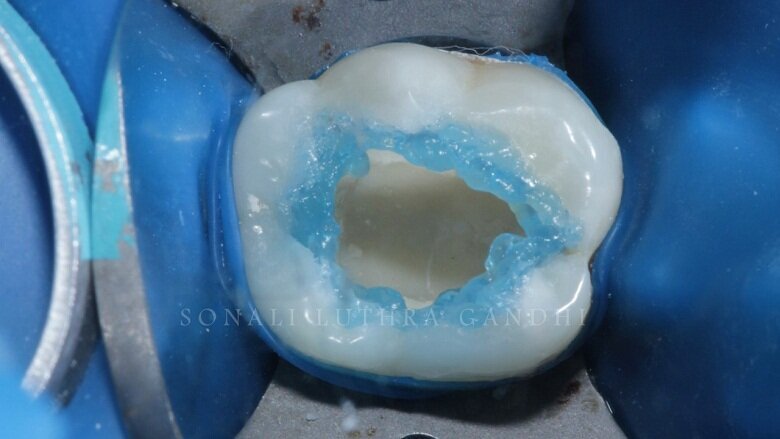
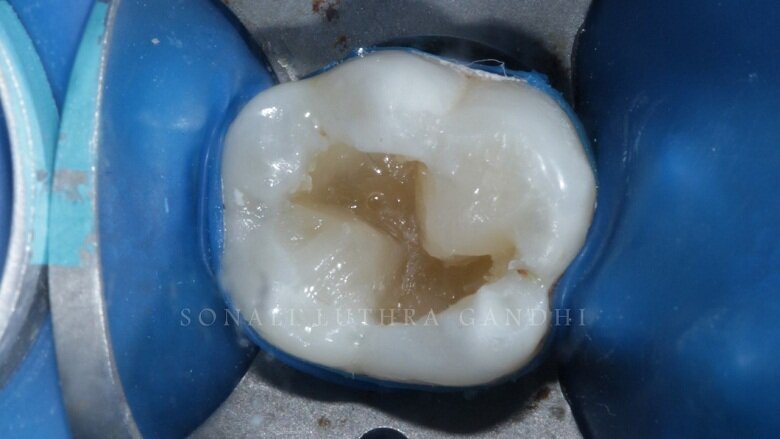
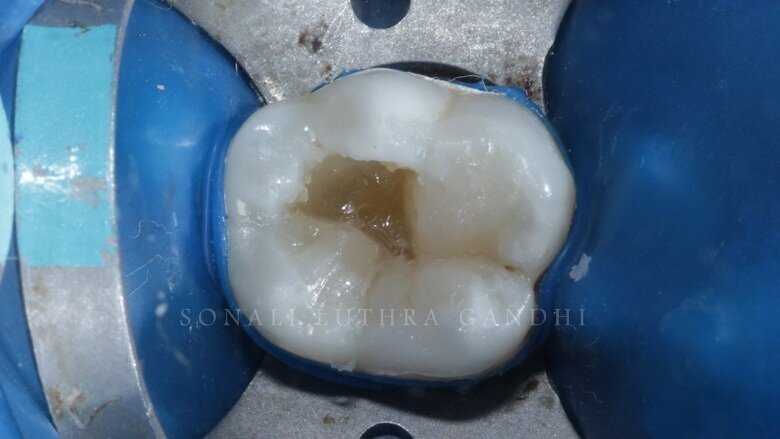
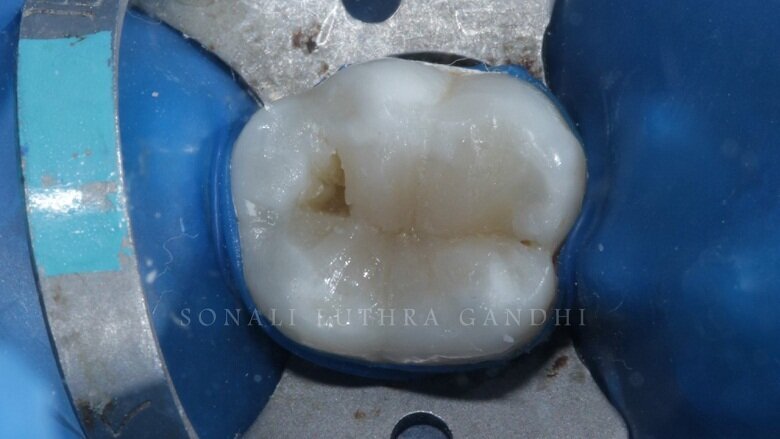
The tooth was then endodontically treated and restored with a non-eugenol temporary cement (Fig. 1). Since the access was only from the center of the tooth only 36 was isolated. The tooth was isolated with the help of a rubber dam (Fig. 2). The temporary restoration was then removed and the floor of the pulp chamber along the gutta percha points were visible (Fig. 3). This floor was then sealed with resin modified glass ionomer cement (RMGIC) (Vitrebond, 3M) and cured for 40 seconds (Fig. 4). This step is extremely important so as to protect any seepage of any material into the canals.
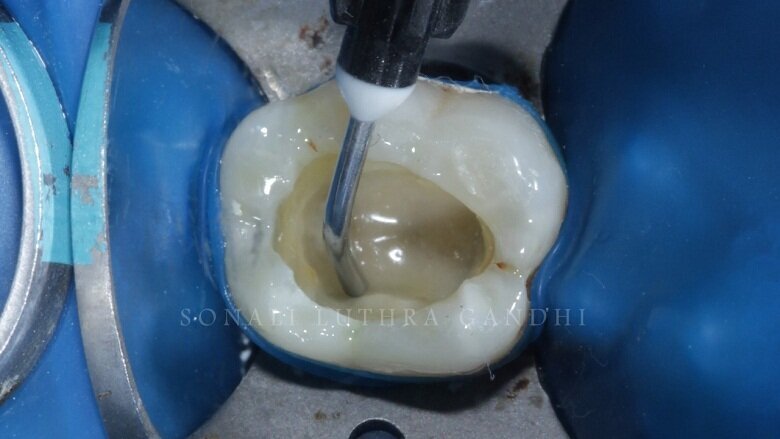
Once the orifices were sealed the restorative procedure was started. The first step is to introduce the first solution i.e etchant. The cavity was now conditioned with 37% phosphoric acid for 30 seconds only in the enamel layer. (Fig. 5) The dentin was not subjected to the etchant thereby following the selective etching protocol. The cavity was thoroughly rinsed and air dried. The dentin bonding agent was applied (self-etch adhesive, 3M/ESPE), gently air dried to evaporate the solvent, and light cured for 20 seconds (Fig. 6).
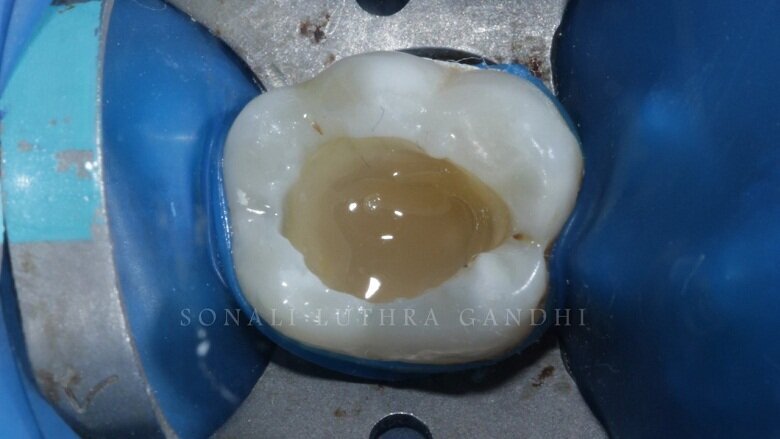
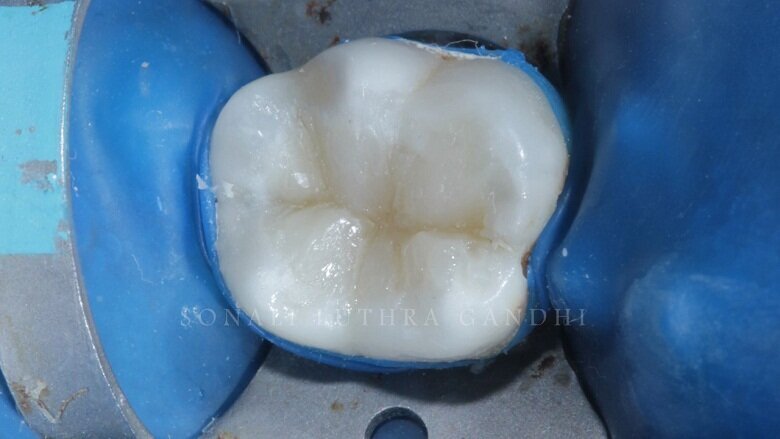
A layer of A2 (3M Flowable composite) flowable composite was then placed on the base for reducing the polymerization shrinkage stresses (Fig. 7). The cavity is now ready for the composite restoration (Fig. 8). The shade selected in this case is A2 (3M Filtek Z350 XT). The cuspal layering technique will be applied here.
To follow this procedure,the anatomy of the tooth to be restored must be known thoroughly. In this case the tooth is a lower first molar. It consists of three buccal: - mesio-buccal, disto-buccal, distal cusp and two lingual: - mesio-lingual and disto-lingual cusps. The most important element is the central fossa, as this is the starting point of all the functional movements. The tip of the mesio-palatal cusp of the first upper molar interdigitates with the central fossa of the first lower molar.
After positioning the central fossa we must imagine all the functional movements. The first increment of the composite is used to reproduce the mesio-buccal cusp (Fig. 9). Light cured for 20 seconds. Each layer must be perfectly adapted to the margin of the preparation in order to prevent time wasting finishing adjustments.
The next cusp is the disto-lingual cusp which is diagonally opposite to the first cusp (Fig. 10). There is no specific pattern for building the cusps but building diagonally opposite cusps helps to determine the central fossa better. This increment is then light cured for 20 seconds.
The next in line is the mesio-lingual cusp. Small secondary fissures are given while layering to give a more natural anatomic appearance (Fig. 11), which is then light cured for 20 seconds. With this increment completed the lingual anatomy is now built completely which is followed by the buccal anatomy. The disto-buccal cusp is now placed (Fig. 12) and light cured for 20 seconds.
The key point to remember is that while layering every cusp to leave a sharp groove between the two increments to resembles fissures in which tints can be flown. These sharp groves define the anatomy and give a crisp appearance of the cusps differentiating each cusp from the other. The smallest of all the cusps i.e the distal cusp is now layered, flushed with the margins and light cured for 20 seconds (Fig. 13).
Tints are placed into the grooves very artistically starting from the central fossa (Fig. 14). This is also light cured for 20 seconds. After this an oxygen barrier solution is applied and light cured through this layer for 20 seconds. The dam is removed. Occlusion is checked and adjusted.
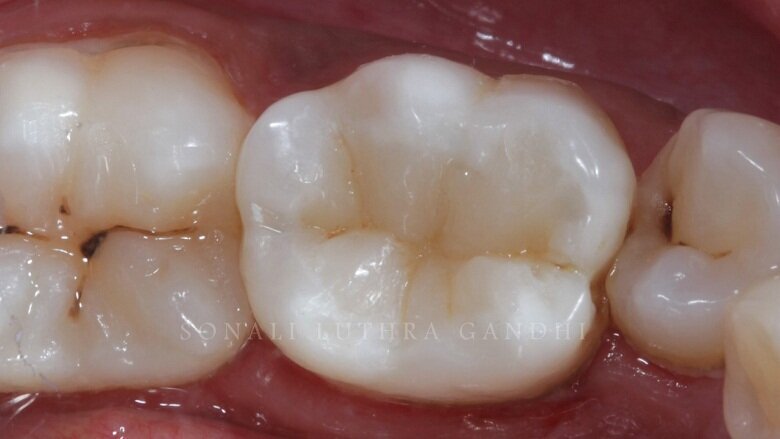
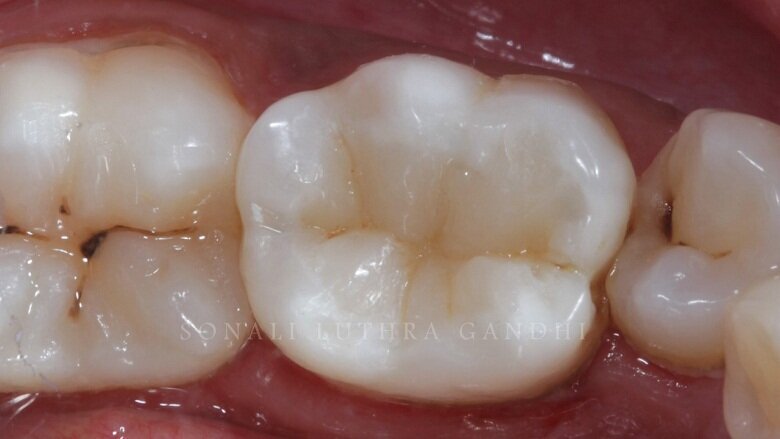
The restoration is now finished and polished with the help of finishing burs and discs (3M Soflex Spirals) followed by a series of buffs with a polishing paste. The restoration is now completed (Fig. 15).
Conclusion
Direct composite restorations have become a pivotal part of the active dental practice. Methods to upgrade efficiency and speed of their placement should be incorporated with the objective of long-lasting and properly formed restorations.The occlusal scheme, preparation of the remaining tooth structure, and remaining dentin thickness are all considerations that play an important role in the prognosis of the restored tooth.
After assessing these factors, the clinician should choose a restorative technique that aims to minimize the stress created by polymerization shrinkage, establish an ideal occlusion, and protect the pulpal complex. This approach will reduce the chances for postoperative sensitivity, marginal enamel fractures, premature marginal breakdown, and pulpal injury and thereby will increase the longevity of the restoration.
Fig 1: Pre-operative photograph
Fig 2: Isolation achieved with Rubber Dam
Fig 3: Removal of temporary restoration
Fig 4: Orifices sealed with RMGIC
Fig 6: Application of Self etch Bond
Fig 7: Application of Flowable Composite
Fig 8: Ready for composite restoration
Fig 9: Cuspal Build up Technique – Mesio-buccal cusp
Fig 10: Disto-lingual Cusp
Fig 11: Mesio-lingual Cusp
Fig 12: Disto-buccal Cusp
Fig 14: Application Of Tints



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East













































To post a reply please login or register