The last decade has witnessed a global rise in antibiotic resistance, creating substantial challenges for healthcare systems worldwide. While the primary focus has traditionally been on comprehending the impact of antibiotic usage on resistance development, a novel concept in microbial ecology is unveiling the potential role of the human oral microbiome in the spread of antibiotic-resistance genes. This concept, termed the “Oral Resistome” delves into the complex interplay between the oral microbiota and the acquisition and transfer of resistance genes. In this article, we explore the world of oral resistomes, their connection to dental diseases, and antibiotic profiling.
Oral resistome: An emerging concept
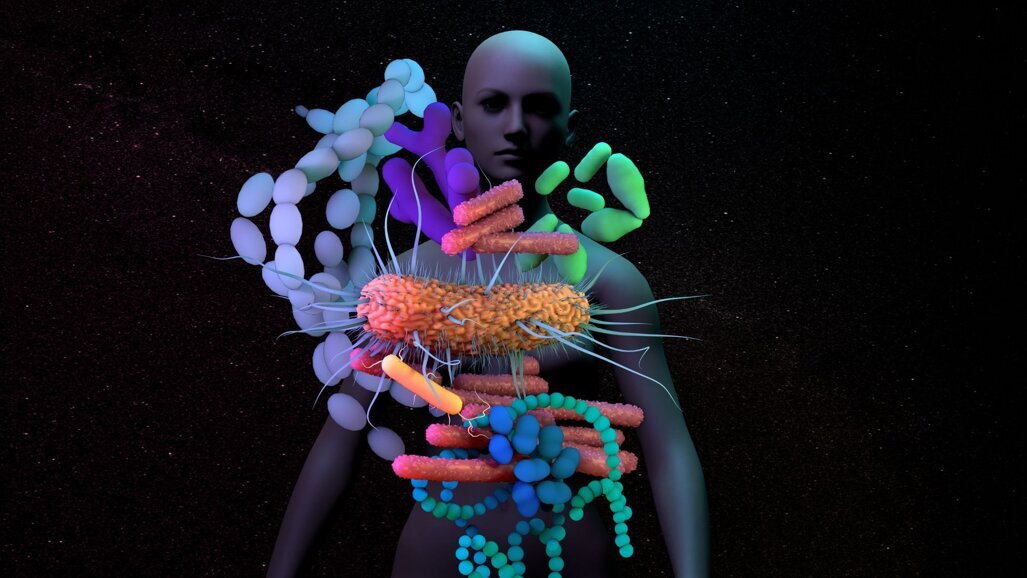
The oral microbiome is the second-largest microbial community in the body, after the gut. 1
The oral resistome refers to the collection of antibiotic-resistance genes (ARGs) present in the microbial community of the oral cavity. It encompasses the genetic material that can confer resistance to antibiotics and is carried by various microorganisms inhabiting the oral environment. 1
Oral resistome can provide valuable insights into screening and managing dental diseases. Here’s how.
- Early resistance detection: Screening the oral resistome may enable for the early discovery of antibiotic resistance in oral infections. Dentists can spot rising resistance patterns and alter treatment methods by tracking the prevalence of resistance genes over time.
- Screening high-risk populations: The oral resistome analysis can aid in the identification of certain patient populations or subgroups who are more likely to harbor antibiotic-resistant oral bacteria. This information can help prioritize screening efforts and execute preventative measures in people who are at higher risk, such as those with impaired immune systems, chronic diseases, or a history of antibiotic usage.
- Personalized therapy: Antibiotic therapy for dental disorders can be improved by having a better understanding of the oral resistome. Clinicians can choose medicines that are more likely to be successful against the most common resistant strains by recognizing the antibiotic resistance genes dominant in an individual. This individualized strategy can improve treatment results, lower the risk of antibiotic resistance, and cut down on the overuse of antibiotics.
- More efficient antimicrobial prophylaxis: Invasive dental treatment in high-risk patients needs prior antibiotic prophylaxis. Understanding the oral resistome can guide the development of evidence-based guidelines for resistome-specific antimicrobial prophylaxis. This will ensure that appropriate antibiotics are prescribed while minimizing the risk of promoting further resistance.
Understanding the oral microbiome changes with age: The milestones
Oral resistomes, a crucial part of the oral human microbiome, include a reserve of ARGs that are directly linked to the ever-growing threat of global antimicrobial resistance (AMR).1
Given the fact that the oral resistome builds upon the oral microbiome, we must take a look into the age-wise evolution of the oral microbiome.
The age-old belief is that oral microbial colonization occurs after birth (the sterile womb concept). However, current research has confirmed that the human microbiome begins to develop before birth. The oral bacterial diversity continues to evolve through time.2,3 Diet, genes, the eruption of teeth, habits, and environmental factors bring about these alterations. Here is an age-wise mapping of the oral microbiome in newborns, during the first year of their lives.
- Prenatal: Interestingly, amniotic fluid from up to 70% of pregnant women includes several oral microorganisms, such as Streptococcus, Fusobacterium, Neisseria, Prevotella, and Porphyromonas. Instead of the gut microbiome, the placental microbiome is more similar to the pregnant mother's mouth microbiome.3 Simply put, the maternal oral microbiome directly influences the newborn oral microbiome.
- 0-6 months: Just after birth, a newborn is exposed to a broad variety of microorganisms, via diverse contact routes. The early colonizers include bacteria, fungi, parasites, and viruses. The majority of these are Gram-positive facultative, followed by Gram-negative anaerobes. Among the oral fungi, Candida remains abundant from the first day, and throughout the first year.2
- 6 months to 1 year: The oral ecosystem undergoes changes when the first primary tooth emerges- there is a decrease in the presence of Gram-positive facultative bacteria and an increase in Gram-negative facultative bacteria. One specific example is Streptococcus mutans, which rapidly colonizes the oral cavity during this stage with the newly erupted teeth as their preferred surface for adhesion. With the emergence of teeth, plaque microbiota also comes into existence and forms a distinct oral community. By this time, Veillonella, Streptococcus, Actinomyces, Selenomonas, and Leptotrichia make up the most abundant genera.2
- 1 to 5 years: Pediatric oral resistome is an inherent feature of the oral microbiome from infancy, which develops throughout childhood. As the child grows, crucial changes like the transition from primary to mixed to permanent detentions, diet changes, hormonal changes during adolescence, and changes in host immunity add up to create a more diverse oral microbiota. This diversity increases in the first few years of life before it is stabilized at around age five.2
These milestones are the stepping stones for characterizing the AMR potential of the human oral microbiota.
Is oral resistome a mirror of health and disease?
Accumulating evidence now highlight that the oral resistome has the potential to mirror the state of health and disease.3 Taking a step ahead, studies are acknowledging oral resistome as a novel screening tool for dental diseases.
Let's look at some groundbreaking studies.
A first-of-its-kind study4 aimed to determine whether the oral microbiota represents a source of ARGs and how the resistome differs in healthy (H) individuals as compared to caries active (C) individuals and chronic periodontitis (P) patients. The shotgun metagenomics sequencing combined with the culture technique was used to generate comprehensive data on the microbiome and resistome.
The team found 64 ARGs conveying resistance to 36 common antibiotics, particularly to tetracycline, macrolide-lincosamide-streptogramin, and beta-lactam antibiotics. Interestingly, based on the microbiota composition, these ARGs cluster in different resistotypes, and a higher prevalence is found in healthy and caries active than in periodontally diseased individuals. The ARGs with the highest prevalence in healthy and caries-active individuals were mefA, msrD, cfxA, and ermF, and tetQ, pgpB, and tet32 in periodontitis. The species that most commonly possessed ARGs were Streptococcus mitis, P. gingivalis (20.9%), P.intermedia (15.8%), L. wadei (11.3%), and Gemella oral taxon 928 (6.2%).
The experts concluded that “Interestingly, significantly fewer ARGs were detected in P than in H and C, which can be explained by the lower diversity and differing microbial composition in periodontitis. The oral microbiome is a rich reservoir for multiple ARGs which can be clustered into different resistotypes based on the specific differences in the microbiota composition and also depending on the respective condition of the individuals, i.e. health, caries, or periodontitis.”
Keeping in mind the potential implications of this study, the researchers quoted that given these findings and the proof that antibiotics are frequently prescribed in dentistry without an appropriate indication, prudent antibiotic use is highly advised, and additional study is required to clarify any potential horizontal gene transfer and spread of resistance through oral bacteria.
Another recent study investigated if the resistome composition changes in a disease condition (caries). The team looked at variations in overall resistome abundance and diversity between the caries-free (CF) and caries-active (CA) groups. Results showed discrepancies at the ARG level. The CF resistome has 83 ARGs compared to 57 ARGs in the CA resistome, with 15 common ARGs.
In all groups, the most abundant AMR gene class was macrolide resistance followed by beta-lactams. The severe category (ICDAS Classification) had the highest compositional change in microbiome, resistome, and insertion sequences. Interestingly, the team highlighted that BlaOXA-85, associated with health, was significantly more abundant in resistomes of children who had restorations-suggesting that the placement of a restoration favors a return to microbial homeostasis.1
Takeaway
Throughout human history, antimicrobial resistance genes have been identified in the oral microbiome and have been detected in people of all ages, from neonates to adults. However, their potential effect on dental diseases and how to treat them is, is gaining traction only recently. Deciphering these oral resistomes holds immense potential to transform the way we screen, diagnose, and manage dental diseases. Resistomes can be the stepping stone towards personalized dental treatments, effective infection control strategies, and a future where antibiotic resistance is tamed!
References
- Sukumar, S., Wang, F., Simpson, C.A. et al. Development of the oral resistome during the first decade of life. Nat Commun 14, 1291 (2023). https://doi.org/10.1038/s41467-023-36781-w
- Kahharova, D., & Zaura, E. (2021). Acquisition and establishment of the oral microbiota. Periodontology 2000, 86(1), 123-141. https://doi.org/10.1111/prd.12366
- Xiao, J., Fiscella, K.A. & Gill, S.R. Oral microbiome: possible harbinger er for children’s health. Int J Oral Sci 12, 12 (2020). https://doi.org/10.1038/s41368-020-0082-x
- Anderson AC, von Ohle C, Frese C, Boutin S, Bridson C, Schoilew K, Peikert SA, Hellwig E, Pelz K, Wittmer A, Wolff D, Al-Ahmad A. The oral microbiota is a reservoir for antimicrobial resistance: resistome and phenotypic resistance characteristics of oral biofilm in health, caries, and periodontitis. Ann Clin Microbiol Antimicrob. 2023 May 13;22(1):37. doi: 10.1186/s12941-023-00585-z. PMID: 37179329; PMCID: PMC10183135.
Tags:
The crisis of antimicrobial resistance (AMR) stems largely from the widespread misuse and overprescription of antibiotics across various sectors, including ...
This article explores how artificial intelligence and augmented reality are revolutionising cosmetic dentistry—especially, how virtual smile previews help...
LISBON, Portugal: Technological progress is not only helping the development of newer implant treatment techniques but also creating a need to update the ...
Bangalore, India: Prof. Dr.Girish Rao S is a renowned Oral and Maxillofacial surgeon. He is the founder mentor of Implant Study group which conducts one of ...
Vitamin D is a steroid hormone that is obtained through diet or synthesised in the skin from cholesterol when the skin receives adequate sun exposure (the ...
Dr. Isha Rao writes about FDI’s Global Antimicrobial Research Dental Network for Early Career Researchers (GARD ECR network) studying this field. The ...
PHILADELPHIA, U.S.: Some young children experience severe dental caries that resists normal therapies. According to a recent study carried out by ...
The next time you flash a smile, remember — a small part of it might be Neanderthal.
Why do some people have broader, stronger teeth, while others have ...
STOCKHOLM, Sweden: Antibiotic resistance as a result of overprescription is a topic of great concern for researchers and activists across all specialties ...
MILAN, Italy: Since the evidence of oral manifestations linked to SARS-CoV-2 is scarce, researchers have recently set out to fill the gap by investigating ...
Live webinar
Wed. 3 June 2026
10:30 pm IST (New Delhi)
Live webinar
Thu. 4 June 2026
11:30 pm IST (New Delhi)
Live webinar
Mon. 8 June 2026
9:30 pm IST (New Delhi)
Live webinar
Mon. 8 June 2026
10:30 pm IST (New Delhi)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
11:30 pm IST (New Delhi)
Live webinar
Wed. 10 June 2026
8:30 pm IST (New Delhi)
Live webinar
Wed. 10 June 2026
11:30 pm IST (New Delhi)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East

















































To post a reply please login or register