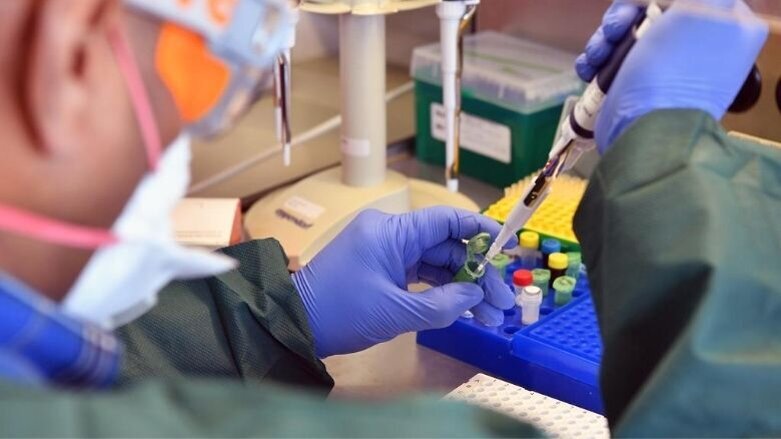
Currently, all SARS-CoV-2 detection measures make use of RT-PCR test, and its results are generally reported as either positive or negative, which tells us if a person is infected. However, to contain the pandemic, what we need to know is whether that person is infectious or in other words, 'can he spread the disease?' It's important to know that the RT-PCR test does provide an additional measure of the viral load in the sample. This reading is called the cycle threshold (Ct) value. Evidence suggests that reporting this Ct value (calculated viral load) can assist in a better interpretation of the condition, and also in taking clinical decisions.
Our main objective is to prevent the spread of COVID-19 pandemic, for which we must identify and isolate infectious people. Hence, it is critical that those with a high viral load are isolated and not allowed to transmit the virus to others.
Quantitative vs Qualitative data
Currently, all detection measures viz. diagnosis, screening, and surveillance depend on a reverse transcriptase–quantitative polymerase chain reaction (RT-qPCR) test, and we report its results as either positive or negative.
However, it's essential to know that the RT-PCR test does provide a measure of the viral load in the sample, and the reading is called the cycle threshold (Ct) value. Evidence suggests that reporting this Ct value (calculated viral load) can assist in the better interpretation of the condition and support the clinical decisions.
Measuring infectivity by viral culture
RT-PCR testing can tell us whether there is a detectable virus present in an individual. Still, it does not accurately tell us whether that individual is infectious or is capable of spreading the disease. Infectivity in cell culture is the standard for determining whether a patient is contagious.
In the absence of viral culture data, one can use viral load or cycle threshold (Ct) values derived from RT-PCR as a proxy for the likelihood of transmission. The Ct is the number of replication cycles required for a signal of RT-PCR product to cross a determined threshold.
Early studies on symptoms and viral shedding
Early studies showed the highest viral load in throat swabs at the time of symptom onset and inferred that infectiousness peaked on or before symptom onset.
Another early study showed pharyngeal virus shedding to be very high during the first week of symptoms, with a peak happening on day 4.
Correlation between symptoms and Ct values: (JAMA Internal Medicine, 6 Aug 2020)
In this cohort study, both asymptomatic and symptomatic SARS-CoV-2 patients showed similar Ct values. Viral molecular shedding was prolonged. Since asymptomatic/ presymptomatic transmission of SARS-CoV-2 infection may be a critical factor in community spread, population-based surveillance and isolation of asymptomatic patients may be required.
Infectivity: Ct values & viral culture
In a German study (click here to read) the researchers could readily isolate the virus during the first week of symptoms from a significant fraction of samples. Still, no isolates were obtained from samples taken after day eight despite ongoing high viral loads. The study recommended an early discharge with ensuing home isolation for patients who are beyond day 10 of symptoms with less than 100,000 viral RNA copies per ml of sputum. Both criteria predict that there is a little residual risk of infectivity, based on cell culture.
In a French study published in April 2020, the researchers at the Méditerranée Infection University Hospital Institute in Marseille, France collected 183 samples from 155 patients. Out of the 183 samples obtained, 174 were nasopharyngeal swabs, and 9 were sputum samples. They assessed the patient samples for SARS-CoV-2 RNA positivity using real-time RT-PCR targeting the E gene. All 183 samples were inoculated in cell cultures. The objective was to correlate viral load to cultivable viruses.
Among the 183 samples inoculated in the studied period, 129 led to virus isolation. Of these, 124 samples had detectable cytopathic effect between 24 and 96 h. Blind subcultures allowed obtaining five additional isolates only.
The study found a significant relationship between Ct value and culture positivity rate.
- Samples with Ct values of 13–17 all led to a positive culture.
- Culture positivity rate then decreased progressively according to Ct values to reach 12% at 33 Ct.
- No culture was obtained from samples with Ct > 34.
- The five additional isolates obtained after blind subcultures had Ct between 27 and 34 (low viable virus load).
Thus the study found a strong correlation between Ct value and sample infectivity in a cell culture model. The authors could deduce that with this system, patients with Ct values equal or above 34 do not excrete infectious viral particles.
A study done in Manitoba (May 2020) evaluated the relationship between cycle threshold (Ct) values (wrt E gene SARS-CoV-2 RT-PCR from respiratory samples), symptom onset to test (STT) and infectivity in cell culture. They took SARS-CoV-2 RT-PCR confirmed positive samples and determined their ability to infect Vero cell lines. The study observed no growth in samples with a Ct > 24 or STT > 8 days. The authors concluded that the infectivity of patients with Ct >24 and the duration of symptoms >8 days might be low.
For every 1 unit increase in Ct, the odds ratio for infectivity decreased by 32%. The high specificity of Ct and STT suggests that Ct values greater than 24, along with the duration of symptoms lasting longer than eight days may be used in combination to determine the period of infectivity in patients.
Contrary evidence
One study, published in the NEJM in May 2020, coming from a skilled nursing facility in Kings County, Washington, found viral growth in a patient sample with a cycle threshold (Ct) value of 34, as well as viral growth in asymptomatic and presymptomatic individuals. However, a systematic review from Stanford University analysing this study said that the findings from an elder care facility might not reflect the general population. Reasons are two-fold.
- It is difficult to recognise early signs and symptoms of respiratory viral infections in the elderly
populations due to impaired immune responses associated with ageing and the high prevalence of pre-existing and underlying conditions, such as chronic cough and cognitive impairments.
- Elderly and infirm patients have blunted physiological responses that may allow them to remain asymptomatic during infection.
Latest systematic review (21 Aug 2020)
The latest systematic review on this topic MedRxiv, 21 Aug 2020 included 17 studies that suggested a correlation between the time from collection of a specimen to test, cycle threshold (as a proxy for viral load) and symptom severity. The quality of the studies was moderate with lack of standardised reporting and lack of testing of PCR against viral culture or infectivity in animals limiting our current ability to quantify the relationship between the variables and ultimately the usefulness of PCR use for assessing infectiousness of patients. However, the authors mention that the infectivity appeared to decline after about a week of viral shedding around the cycle threshold value of 24.
BETHESDA, Md., U.S.: COVID-19 can cause a number of symptoms in the oral cavity, such as lesions, ulcerations and a loss of taste, and yet the role of the ...
ChairsideCAD, available from exocad, is the choice of software for leading manufacturers of dental CAD/CAM systems, according to the company, and it has ...
Sandeep Chakraborty (B-Tech, Electrical Engineering IIT Kharagpur, 1997), (Masters. Computer science, IIT Kharagpur, 2008) is a researcher focused on ...
The World Health Organization (WHO) updated its communication on the airborne transmission of SARS-CoV-2 on 30 April 2021.
This article summarizes their ...
Several media reports have come up with scary headlines that the new SARS-CoV-2 variants are fooling the RT-PCR test, which is considered the gold standard ...
Dentists and dental patients are showing an ever-increasing concern about the generation of virus-containing aerosols through various dental procedures, and...
Two updates (Sept 18 & 21, 2020) by the Centers for Disease Control & Prevention (CDC) on Covid-19 guidelines, which are relevant to dental practice.
In this article, we analyze four recent articles published in Aug-Sept 2020 on the genetic diversity of SARS-CoV-2 and the potential therapeutic targets ...
NEW YORK, U.S.: In 2019, the Centers for Disease Control and Prevention (CDC) released a statement declaring that Candida auris is an emerging fungus that ...
The human body consists of distinct and abundant microorganisms referred to as the microbiome [1]. The oral cavity is colonized by 700 different species of ...
Live webinar
Wed. 3 June 2026
10:30 pm IST (New Delhi)
Live webinar
Thu. 4 June 2026
11:30 pm IST (New Delhi)
Live webinar
Mon. 8 June 2026
9:30 pm IST (New Delhi)
Live webinar
Mon. 8 June 2026
10:30 pm IST (New Delhi)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
11:30 pm IST (New Delhi)
Live webinar
Wed. 10 June 2026
8:30 pm IST (New Delhi)
Live webinar
Wed. 10 June 2026
11:30 pm IST (New Delhi)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East
















































N Gene 23.91
E Gene 22.82
ORF-1ab 24.73 can you please share the risk level
My sister age is 37 year, she is Covid +ve report yesterday and her orf gene(ct) is 12 N gene(ct) is 13 and S gene(ct) is 13. So can you please let me know how much she is infected and what is the risk level?
My father’s age is 78 year he had his Covid19 report yesterday and his N gene(ct) is 20 and orf gene(ct) is 24 so may you please let me know how much infected he is and how much he is at risk
ORF1ab Detected (CT-31)
N gene Detected (CT-32)
HOW MUCH INFECTED RISK AND HOW MUCH IS AT RISK
MY AGE 48, I AM DIABTIC
I AM USING GLADOR M1, AND TGLIP, GLORISTAT
My father’s age is 53 year he had his Covid19 report yesterday and his N gene(ct) is 24 and orf gene(ct) is 25 so may you please let me know how much infected he is and how much he is at risk
What it means ct 23 and how many moredays of home isolatio and when I do new pcr test my age 80 years
My ct value is 23 what it means and what is the estimated time to quorantine isolate at home my age is 81 years very mild symptoms
pl.how to take care of patient.
what is real treatment.
My ct value is 23 what it means.
My Rt pcr done on 25 dec. Result on 26dec. Ct value 20. It is low risk or high risk. N gane and S gane they write “Detected ” . Pl give me reply. Thanks
if CT is 17.49 is it low or high risk
If CT value is 27.71 is high or low risk
My N-Gene ct value is 33 and ORF1 ab-gene ct value is 31
test 13.12.20.i am 68 years old. No symptom other than cough which is chronic.
How to interpret it.
MY CT VALUE IS 36 AFTER 18 DAYS OF FIRST TEST WHEN MY CT VALUE IS 19.
PLEASE SUGGEST SEVERITY OF DISEASE.
My name is Ritu Patel
Postive on 20th nov 2020 ct value (32)and after 14 days reports are this
ORF 1ab Gene : * TARGET DETECTED
N gene : * TARGET DETECTED
Conclusion : * COVID-19 POSITIVE (CT VALUE: 28-29 )
How many days to recover for nagative?
My wife sangeeta is admitted in bkc covid centre at phase 2 , CKD.
JUST NOW I got her rt CPR report is positive.
ORF 1ad gen is 23.4
N gene is 25.62
I am very frightened. Please explain me what is condition of patient. Is she out of danger.
E gene Ct value 25.14 and RdRp gene Ct value 26.96 with Positive result. I am 52years old male. I have no any type problem with my body. Now I what to do for Negative. Is it high or low risk. Please guide me. Thanks.
E gene Ct value 25.14
RdRp gene Ct Value 26.96
With result Positive
Now i have no any type problem with my body.what I do for Negative report. Is it high or low risk. Please guide me
N- Gene ct value is 18
ORF1ab- Gene ct value is 18
Age 46 male
Please advice
N gene(ct value) 22.83
ORF 1ab(ct value) 21.72
My report pls tell me low or high virus
Sir
My age is 37 years
My report Target Gene CT Value s 31.44%
Covid19 is detected
Same is done from Throcare
Please confirm this is normal or Middle or High range
my E gene is 24, orflab is 25, N gene is 26 what it mean
On 5th Nov,2020 tested with Covid Positive with ct 19 and now on 21st again tested with Covid Positive with ct 30. Now, when I have to test again for negative
N gene(ct value)15
ORF 1ab(ct value)15
S gene(ct value). 16
My report pls tell me law or high virus
N gene(ct value)15
ORF 1ab(ct value)15
S gene(ct value). 16
It is low or strong
Ct VALUES
SARS-COV2 (COVID-19 Virus) QUALITATIVE, REAL TIME PCR POSITIVE E GENE :32.9
RdRp + N GENE :33.6
It is low or strong ??
My N gene CT Value is 19.82 and ORF1ab gene CT value is 17.21. my age is 35 i got positive report.
pls advise
If my COVID -19 RNA VIRUS PCR
Screening (E gene) Ct Value Confirmatory (RdRp & N gene) Ct Value
POSITIVE (LOW VIRAL LOAD)
24.95 26.75
Negative
RT-PCR
and my age is 56 what is it , I kno it’s a low virus detected and non communicable but what are the risk factors
Need to know E gene and N gene meaning and calculation . What is CT value . Is this sum of E gen and N gene CT VALUE
E Gene 12.450
N Gene\RDRP 13.380
My ct values is 18 advice
ORF 1ab 33,
N Gene 35,
E Gene 34
After 16 days I don’t have any symtoms. What is the meaning of this CT value?
I was tested positive on 5th August & negative on 13th August discharge on 15th August now on 13th November I again tested positive with CT value of 26 with no symptom is I can spread the desees or not & what medication I take
i was negative in rtpcr but still have irritation in throat and whhezing while breathing
My E gene 23
ORF 1ab 25
N gene 25
What is my ct value
My ct values are as follows-
N-Gene=34
E-Gene=34
ORF 1ab=33
What do I do? I don’t have any other symptoms except partial smell loss.
My husband N- Gene ct value is 31:00 & CRF- 1ab ct value is 29:00 what is the meaning of this value
My E GENE Ct VALUE is 24 and RdRp GENE Ct VALUE is 26. Would like to know about infection levels and what is the possibility of spreading this virus to my family. Don’t have any problem with me.
You can find more about the CT values here:
https://www.who.int/diagnostics_laboratory/eual/eul_0515_202_00_covid19_coronavirus_real_time_pcr_kit_ifu.pdf?ua=1
Refer to page# 16.
My mother is covid positive with CT 24.5 ..which stage of covid indicates this value
On 10th Nov my rt PCR count is 27
Is it high viral load or I have to be quarantine
I am quarantine from last 15 days
my CT value is 15.33(SARS CoV-2 Ct Value 15.33), 1 can I spread the disease among family members and for how many days. what medication I should take…my throat is bad and I have fever about 102.6.
My CT value is 30 can i mixed with my other family members.
Is it safe?
My test report has come today, I am positive & My CT value is 22, what does this mean.
My covid report is negative but my mother and father infected their covid ct is 15.98 for mother her age is 57 and father 16.11 and he is 60 years old. Is this cureable????
MY WIFE AGED 54 HAS BEEN DIAGNOSED COVID POSITIVE TODAY WITH CT VALUE
E Gene 19.270 and
N gene\RDRP 19.450
PLEASE SUGGEST HOW TO DEAL WITH IT
RdRp gene 26.95
E gene 25.94
My husband’s report is positive with N gen ct-16.17 & RDRP
Ct-17.12
IS IT Serious or normal or he can spread that virus
My husband ORF gene 18.33
N gene 19.51
S gene 17.48 is this dangerous r not
My RT PCR report is showing
CT value (RDRP / N gene): 33
CT value (E gene):3
I don’t have any symptoms.
What is my risk if I have already completed 14 days isolation.
Please suggest me whether I can come from isolation.
Answer from Dr Rajeev Chitguppi
If you never developed/ do not have any symptoms, you can discontinue your isolation and other precautions after the 10th day of testing PCR positive. You have already completed 14 days.
My father CT values are n 20 orf1ab 21& s21. His age is 66.admitted to hospital. Please suggest his infectivity and further care to be taken care.
Please guide
My RT PCR report is showing
CT value (RDRP / N gene): 32.54
CT value (E gene):30.83
I don’t have any symptoms.
What is my risk and transferring to others also.
My son’s e gene, n gene and ORF 1ab all are 24 what is intentisity ? Pl send response immediately.
My N-Gene is 33
E-Gene is 32
And ORF 1ab is 32
What about may covid risk is covid infection transfer to Other people or not
E GENE 31; ORF Lab 33; N GENE 33.
Please tell me my ct value and my risk.
my wife 61yrs old, RT PCR value 32. 10th day after detection she has been asked to discharge. what are the possibilities of spreading virus. does she require home quarantine and how many days. what are the chances of repulsion. what is the best practice to stay healthy
My son age 32,was having cold and slight sore throat on 23rdOct.On 24th Oct visited Doctor for medical care.Doctor gave medicines and adviced for Covid 19 test. Result came+be with Ct vaue 26.Pl advice
My father’s e gene ct value was 32.2
And orfla gene ct value is 32
What does that mean, please do answer
My PCR test conducted shows ct value of 18 to. All the three parameters. What does it mean for me a 62 year diabetes
I m 38 years old boy, corona’s symptom (fever & cough) was appeared on 27/09/2020 whereas i was got tested rt PCR on 04/10/2020 and the result was Confirmatory Gene Ct Value :-25. Accordingly, Medicines were prescribed by the Doctor to me on 05/10/2020. I faced Fever continuously till 11/10/2020 and cough till 16/10/2020. Further, i was got tested rt PCR on 21/10/2020 and result is Negative. Sir, my questions are as under:
1) what does its value mean “Confirmatory Gene Ct Value :-25”
2) can i break my isolation period.
my Brother wife was detected as positive with CT value E-Gene- 31.12 And RdRP/N 31.12 and do not have any symptoms. What risk do I have currently and in future?
And My Brother Son corona positive , do not have any symptoms. What risk do I have currently and in future?
I was detected as positive with CT value 32.58 and I do not have any symptoms. What risk do I have currently and in future?
Ct.value is 31 ,no symptoms ,already 7 days have passed is the patient can spread covid now
I have tested for Covid and CT value is observed as >30. What it indicates and how many days it will take to recover.
Past 22 days I tested my covid and it was coming out positive and my ct value is 22 . Then after again 17 days I have tested my covid and found positive .Does I am infectious now?? And what gonna be my ct value no
I do not believe the FDA allows labs to report quantitative data under EUA.
N gene ct value is 28
Orf ct value is 29
For 3 yrs child what does its meaning
N how can we improve the value at home isolation
My CT value is 15 pls reply
My rt pcr test on 15th showed detected (22)
What kind of risk do I have, I do not have any symptoms
यदि E- Gene CT -18 hai aur ORF 1ab bhi 18 hai to kya ye उच्च जोखिम है या निम्न जोखिम है, कृपया बताएं
My ct value is e 19 and n 19.62
Ct value <35…it will be risk or not ?
Target gene=33
E-gene=32
Ct value <35…it will be risk ??
Target gene=33
E-gene=32
My Ct value is 37+
what does it mean when my anti body test is 5,97?
China considers CT value of 40 and above as non-infectious. India considers CT value of 35 as non-infectious
Hi, My name is Kabiraj and I am 62 years male. My PCR test result shows:
SARS-COV-2 (ORF1ab gene) : Detected ( CT Value: 15.18)
SARS-COV-2 (N gene) : Detected ( CT Value: 15.61)
SARS-COV-2 (E gene) : Detected ( CT Value: 15.83)
What it suggests?
I wish they just put the freaking Ct Values in a table with corresponding implications! Dafuq i just read!? i need a Semester of Bio-English terms to understand what they imply…
How can I determine my Ct value from this Real Time RT-PCR positive as N gene-24, ORF-20 and S gene-20?
My CT value 31.83 pl advise
test detected positive
My CT value is 13, what is means
it is high or low
Please answer
If the E-Gene ct value is 31 and orf 1ab-Gene ct value is also 31. What its mean. will this person can spread infection to other family members.
MY grand daughter is 6 Year old
Her PCR Test conducted on 4th October 2020
ORF1ab gene=29.71
N gene = 30.64
E gene = 27.81
How we can safely accompany her
my PCR test conducted on 01th is as under:
N-gen Ct-value =16
E-gen CT-value =16
ORF 1ab CT Value = 16
I am 32 years old, yr answer is expected to how will be my report in negative after how many days. I lost my Smell and taste feeling. Pl Doctor or any suggest me for best results.
my PCR test conducted on 29th is as under:
N-gen Ct-value =16.8
E-gen CT-value =15.6
ORF 1ab CT Value = 16.2
What is the range to be negative and positive , i am 64 years old, yr answer is expected
keep in mind that Ct value is a direct function of the concentration – once you add 100 ng of RNA isolate to the RT reaction – you may get Ct 30; if you start a reaction with 1 microgram – Ct will be shifted to 25, etc. You use commercial positive and negative control samples for gating.
N gene – 23
Orflab -21
S gene – 22
Iwas suffering from respiratory problem since 30th August and got my corona test on 3rd September positive with ctv23 and got admitted in hospital for 15 days during which I was put on oxygen for12 days. After spending 15 days in hospital I am under home quarantine till today for a weak, now I cNnot stand and walk even. For how many days more I would have to remain in isolation from my family. Can still I spread the virus among my family and friends. For how many days it will take me able to see my family or visitors and physiotherapist to provide
me massage or physiotherapy to me
Sir
If n gene 12.85
S gene 12.08
Then what is Ct value
My ct value is 16 whdit is myvstsus
If ct value is 27 and 28 is it high or low infection for person above 50 years
If CT value is 24.20 is high or low risk
My real time PCR report is
N gene(CT) 29
Orf Gene (CT) 28
S gene (CT) 28
So what is my CT value ?
very informative
If ct value is explained visually, it will be more clearer
Clinical reference for this study