Dr Ali Tunkiwala (MDS, Prosthodontics) maintains a dental practice in Mumbai, primarily focused on Implants, Aesthetics and Full Mouth Rehabilitation. He is an accredited member of the American Academy of Cosmetic Dentistry, and also a Fellow and Diplomate of ICOI (International Congress of Oral Implantologists) & ISOI (Indian Society of Oral Implantologists). He is a speaker for the International Team for Implantology (ITI), and also serves on the editorial board of various international journals and periodicals in dentistry. Dr Ali has several peer-reviewed publications to his credit and has authored a chapter in
the book titled, “Graftless Solutions in Implant Dentistry”. He is the Director of “Impart Education”, a continuing education initiative to nurture and guide motivated clinicians towards predictable evidence-based dental practice. In this interview, he talks about three of his favourite topics: Minimally Invasive Dentistry, Esthetic Rehabilitation, and Digital Dentistry.
Since when have you become a strong advocate of minimally invasive dentistry? How different was your practice when you started?
It takes a while for clinicians in practice to decipher that enamel and tooth structure as such, is not a renewable resource. Once cut, it cannot be replaced at all. So, the transformation was gradual for us. In early days, 23 years, ago, when we started work, we had materials that required too much tooth structure to be taken away. Our textbooks recommended taking away close to 1.2 to 1.4 mm tooth structure on labial of anterior, for aesthetic reasons as the material of choice was PFM. That always got us into dentin, where we ended up decreasing the rigidity of the teeth and had far too many structural failures. Over the last decade, advances in ceramic materials and resins have given us the option to prepare teeth lesser and achieve better aesthetic results. Add to that, our understanding of occlusion and other aspects have led to better treatment protocols that are less invasive, and we strive to end up being within enamel at the end of the tooth preparation, as far as possible. If I look back, our practice has totally transformed from trying to make the restorations strong while weakening the teeth, to retaining the strength of teeth with optimally strong restorations.
What are the recent trends that have significantly transformed your practice of full mouth rehabilitation?
The understanding of the interaction between the joints, muscles and teeth have undergone a sea change. We now know that teeth can get destroyed due to parafunction that is brain mediated and may even be damaged due to the acid influx in the oral cavity that may be gastric reflux or consumed as drinks. There is so much in sleep dentistry that is affecting our diagnosis and the overall treatment plans. We understand better what lack of proper sleep and incorrect breathing during sleep can do to our occlusion. Many such aspects have helped us organise our diagnostic capabilities and also allowed us to do a thorough risk assessment to enable us to predict the outcomes of complex treatments more accurately.
Furthermore, technological advances in material science and digital protocols have resulted in increased accuracy and performance. The trend in full mouth rehabilitation today is to destroy teeth as less as possible by avoiding aggressive tooth preps. Additive treatment modalities where indicated with adhesive protocols is the way forward. Even more important is that we learn how to prevent occlusal problems. If we learn to see the early signs of total dental breakdown, we can now initiate a preventive system to help our patient avoid a full mouth rehabilitation in the future. That is where our contribution to humanity will be significant.
You mentioned tooth preparations have changed? What has changed and what is done differently today as compared to yesteryears?
The fundamental reason for any tooth preparation is to make room for the restorative material. The amount of preparation depends on the material chosen. Each material has its minimum requirements of thickness that have to be met so that the material will not fracture in function. In the earlier days, the most aesthetic material was porcelain fused to metal, and that required a horizontal finish line preparation known as a shoulder or rounded shoulder or deep chamfer. These finish lines had an average depth of 1.2mm to 1.4mm and usually led to preparation in dentin. Plus, procedures were undertaken to increase prepared tooth length to provide for resistance form from cohesive preparations. Today materials have changed, and adhesive technology has become very predictable. So, tooth preps have been modified to the traditional concept of knife-edged margins. In yesteryears, these were used on cementum or on amalgam and for full metal crowns. Now we have enough data to show that these types of knife-edged margin designs allow aesthetic materials like lithium disilicate and zirconia to be used with slight modification in lab protocols. In literature variations of these designs have been referred to as Vertical preparations. The advantage these offer is that the chances of being within enamel after tooth preparations are incredibly high and thus better for bonding. The disadvantage is that if the lab leaves a ledge at the margin that is not finished well in the restoration, it can lead to periodontal ill-health. However, in most cases this ill-health is attributed to the violated biologic width and not so much to the type of margin geometry. (Fig 1 to Fig 5)
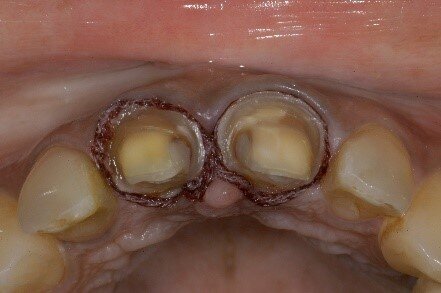
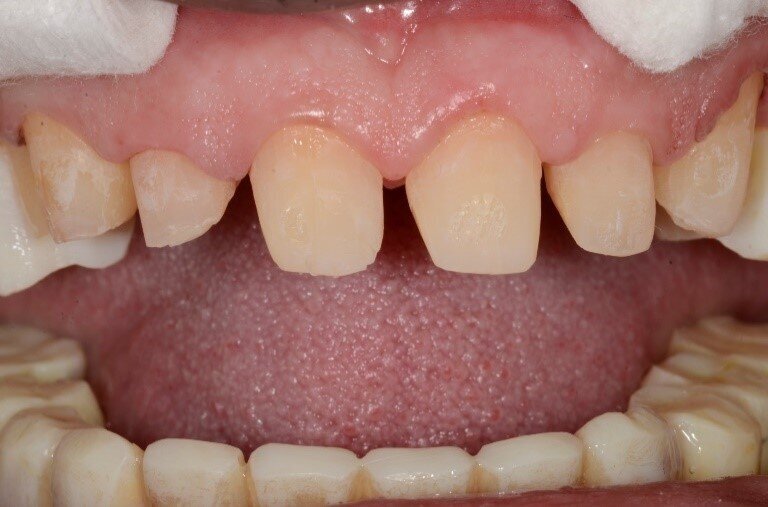
Fig 1: Horizontal margin geometry that requires preparation into dentin
Fig 2: These types of preps can lead to increased flexibility of tooth structure thereby making it prone to breakage
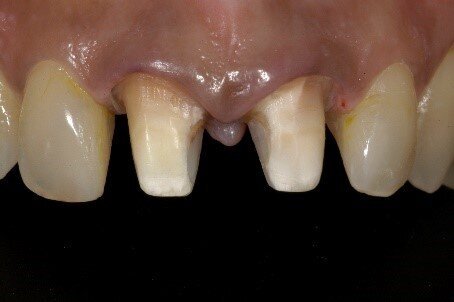
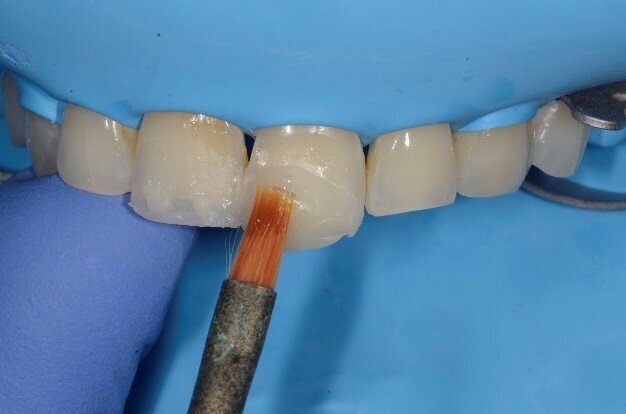
Fig 3: Knife edged margins for lithium disilicate crowns
Fig 4: The presence of frosted enamel all over is a distinct advantage of these margins (Referred to as vertical preps)
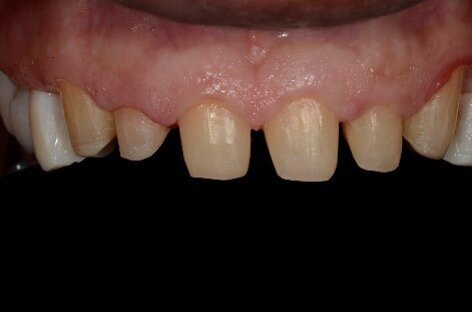
Fig 5: Lithium disilicate restorations bonded and blended well with very fine preparation margins. These restorations offer tremendous benefits as far as pulpal and periodontal health is concerned.
Occlusion is a complex topic to understand and apply in practice. In what way has your practice of aesthetic work changed with respect to occlusion in recent times? If I ask you to give one simple advice to general practitioners, what would that be?
Aesthetics and function are two sides of the same coin. When an aesthetic work is considered to beautify the smile, the functional aspects have to be dealt with in the background to allow the materials to survive in the long term. Hence a clinician who is going to change the anterior teeth, and thereby infringe on the chewing pathway of their patients with veneers/restorations, must start with assessing the need to first carry out an occlusal equilibration. Deprogramming the muscles of mastication to allow an establishment of harmony between the joint and the teeth is paramount. Once the teeth fit well into each other with the joint seated fully in its physiologic space, it will remove any negative stimuli from within the dentition that can lead to stress on the anterior restorations. As a general practitioner, acquiring the skills to deprogram and diagnose the case and then instituting the most conservative methodology of treatment taking into considerations all patient factors like age, health status and habits are of utmost importance. (Fig 6 to Fig 10)
Fig 6: Incisal wear evident and patient complains of slight muscle tenderness.
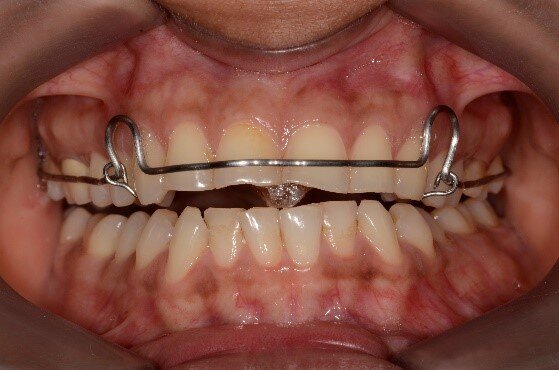
Fig 7: A Kois deprogrammer allows the muscles to relax without the teeth interferences and that helps to the condyles finding their physiologically optimal position within the joint
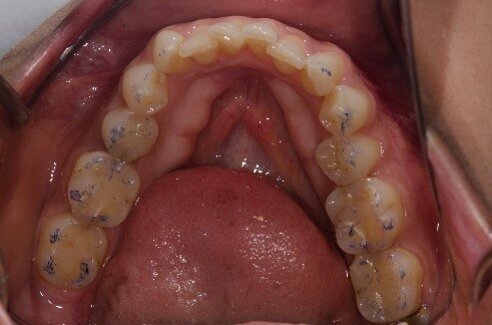
Fig 8: Occlusal equilibration carried out to harmonize contacts on all teeth from canine backwards and adjustments carried out in the end to keep the anterior restorations free from friction in the chewing cycle.
Fig 9: The most conservative treatment modality can then be chosen to restore anterior teeth keeping in mind the age, needs and habits of the patient
Fig 10: The final anterior resin build-ups that now provide the aesthetic solution needed while function was taken care of.
How has digital dentistry transformed your practice in recent times?
The digital revolution has engulfed all aspects of patient care. From Data acquisition in the form of intraoral scanners to virtual designing and articulation of patients’ pre-op data; today everything can be integrated into a digital workflow and true ‘model less’ options are becoming a reality. Integrating the patient's face and dental condition and then seamlessly merging that with the cone beam scan of the patient, a truly holistic pathway can be charted out for the patient's benefits. This not only has a direct bearing on smile design that has become digital, thereby allowing the patient to preview the treatment in totality, but also there has been a huge impact in digital planning for implants with guided surgery. The overall costs of these process have become significantly lower, and the digital protocols that were a privilege of a few big practices are now within reach of a majority of the population. Another aspect is that due to digitisation, data sharing and lab protocols have now a global reach So I can sit in my office and share the patient's data with a surgeon and a lab tech in different parts of the globe and garner the support I need for excellence in dentistry that I like to provide. The world has become accessible to all and thus the way we train and do dentistry has transformed for the better. Digital planning with guided implant surgery, digital planning in orthognathic surgery and orthodontics, digital refinement of occlusion are all possibilities today. There is hardly any aspect of patient care that cannot be done digitally. In these times, clinicians have to be cautious and not get carried away with digitisation on autopilot mode; for the human brain and its contribution to treatment planning is still of great value today and will always be. (Fig 11 to Fig 17)
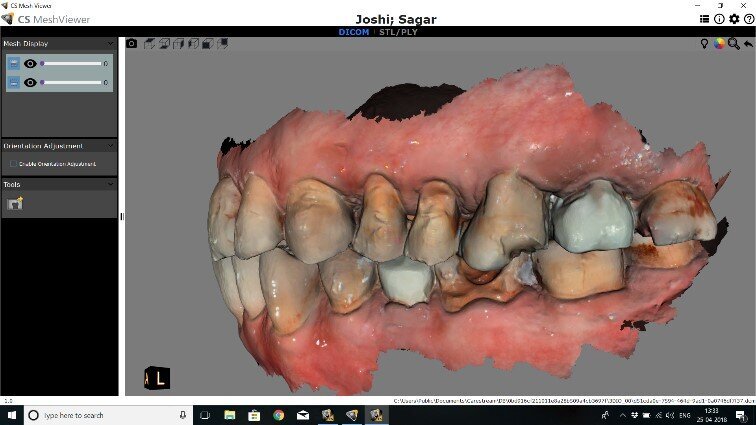
Fig 11: Pre-operative intraoral scans of the patient with severe mutilation of teeth
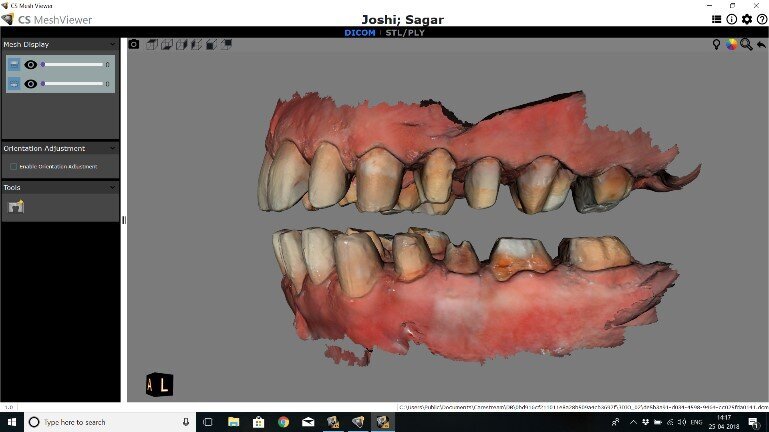
Fig 12: Same patient with digital impressions done for all the tooth preps in the process of a full mouth rehabilitation
Fig 13: The final lithium disilicate restorations bonded in a case that has been done with a full digital protocol.
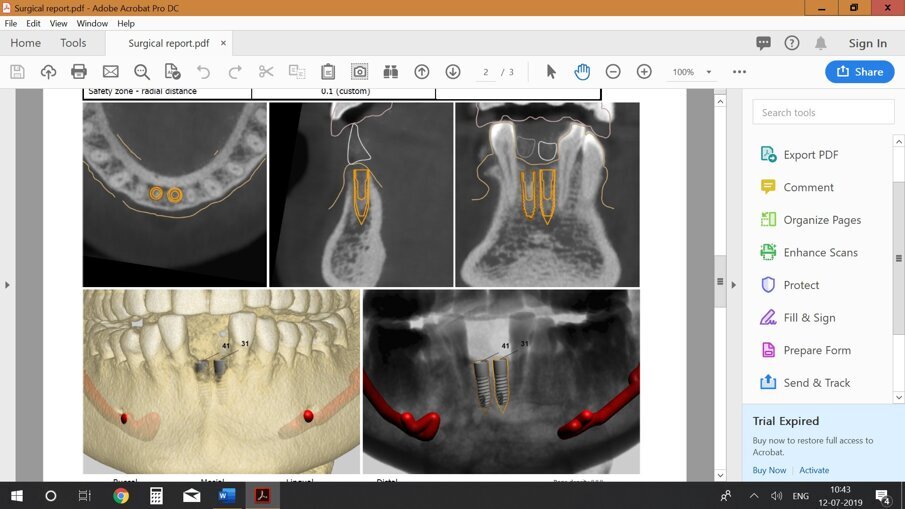
Fig 14: Merging the patients’ pre-operative scanned data with the CBCT data for implant planning.
Fig 15: Digital Planning for implant surgery
Fig 16: Surgical guide used to place implants.
Fig 17: The final restoration on implants placed with guided surgery.
Tags:
Our understanding of soft tissue phenotype around teeth and implants will improve as we utilise novel technologies and advance our knowledge from studying ...
In this monthly column, we interview endodontists and restorative dentists from around the world to share valuable insights with our readers. This month, we...
Two students of grade 11 have developed an AI-based device called the Mouthscope to screen oral cancer and precancerous lesions & conditions, which has ...
Artificial intelligence (AI) has emerged as a game changer in various industries, and oral healthcare is no exception. In recent years, AI has been ...
This article explores how artificial intelligence and augmented reality are revolutionising cosmetic dentistry—especially, how virtual smile previews help...
Dr. Nisha Damle Deshpande interviews Dr. Jordi P. Manauta of Style Italiano for their front-wing technique developed for diastema closure with direct ...
Chennai, India : The 20 Indian Prosthodontic Society (IPS) National post graduate convention was held at Chettinad Dental College, Chennai, on 6 to 8 July ...
Smile Designing doesn’t always have to be about elaborate, extensive and invasive procedures but just sometimes routine procedures done with adherence to ...
MUMBAI, India: As the effects of amalgam fillings on health are still not sufficiently researched, many dentists already rely on alternatives. Cention N is ...
Rapid Antigen Tests are an easy and economical option for dentists to use in their clinics to identify the potential Covid-19 spreaders visiting their ...
Live webinar
Thu. 14 May 2026
9:30 pm IST (New Delhi)
Live webinar
Thu. 14 May 2026
11:30 pm IST (New Delhi)
Prof. Hani Ounsi DDS PhD FICD
Live webinar
Tue. 19 May 2026
8:30 pm IST (New Delhi)
Live webinar
Tue. 19 May 2026
10:30 pm IST (New Delhi)
Prof. Dr. med. dent. Ivo Krejci
Live webinar
Wed. 20 May 2026
4:30 pm IST (New Delhi)
Dr. Graham Carmichael BDSc (Hons), DClinDent (Pros), FRACDS, Dr. Robert Gottlander DDS
Live webinar
Wed. 20 May 2026
6:30 pm IST (New Delhi)
Live webinar
Wed. 20 May 2026
10:30 pm IST (New Delhi)
Prof. Dr. med. dent. Tim Joda PhD, MSc, eMBA



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East






























































To post a reply please login or register